These are the words of Sir Michael Marmot, used 10 years ago, to describe the long shadow cast by health inequalities across the country. Put simply, "inequalities are a matter of life and death, of health and sickness, of well-being and misery"[1]. A decade later and this shadow has darkened, according to the follow-on review released earlier this year (before the world got turned upside down by Covid-19!). Not only have inequalities not improved but, due to austerity policies and other social, economic and political changes, have in fact widened.
Health inequalities arise due to the unequal distribution of social and economic factors which govern how people are born, grow, live, work and age. Whilst access to timely, good quality healthcare is important for good health outcomes, the bigger determinants of a person's long-term health are around early child development, education, good working conditions, enough money to live on and safe, healthy environments to live in.
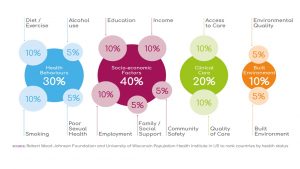
People are not poor with poor health because of bad individual choices. It is that poverty and the restricted choices this presents, along with the associated stress and inadequate conditions, leads to unhealthy actions and worse health.
These wider, social determinants of health cannot be addressed just by ensuring everyone is given the same help and support, as the underlying structures and opportunities disadvantage certain groups. The Marmot reports use the concept of universal proportionalism. This takes the notion of supporting everyone in the same way in an attempt to achieve good outcomes for all (inequalities), to redistributing those resources depending on need (equity) and then to go further in actually addressing the underlying causes to reduce the need in the first place (justice). In other words, tackling the causes of the causes of poor health.

The socioeconomic divide caused by the inequalities and injustice presents a social gradient and a relationship to health, with those in the poorest areas of England dying 7 years earlier than those in the richest. It is not only how long different populations live based on wealth but also how many years of ill health they experience, with those in poorer neighbourhoods spending 17 years more of their already shorter lives in worse health. The situation is not dissimilar across Essex, with a gap between the least and most deprived areas as high as 11 years of life expectancy and 12 years of healthy life expectancy.
The current coronavirus pandemic has shone a light into the shadow of these health inequalities. Far from indiscriminate in its effect on different populations, poorer communities and key front-line workers have borne the brunt of this novel pathogen and the mitigations put in place to slow its spread. As local health & care systems begin to get services and support back up and running after the early lockdown days of the pandemic, there has been clear direction that addressing health inequalities needs to be at the heart of recovery plans.
Whilst it is too early to fully understand the impact Covid-19 has had on the already entrenched inequalities in health, the new health inequalities report produced by the Essex Public Health Intelligence Team, lays out what is already known about the gaps in health outcomes between different groups and communities across the Greater Essex area, and considers the potential impact of the coronavirus pandemic on these health inequalities.
As society reorganises to live with this virus and its effects over the coming months and years, it will begin to understand the true extent the outbreak has had on different population's health outcomes and how, this time, maybe it can get to the root of the inequalities and deliver structural changes to achieve justice.
The Health Inequalities report is available on https://data.essex.gov.uk/
[1] http://www.instituteofhealthequity.org/
Leave a comment